Illicit drug overdose deaths increase in North while other BC regions decline
Northern Health has the highest rate of illicit drug overdose deaths in the province, with the Northeast, Nort…
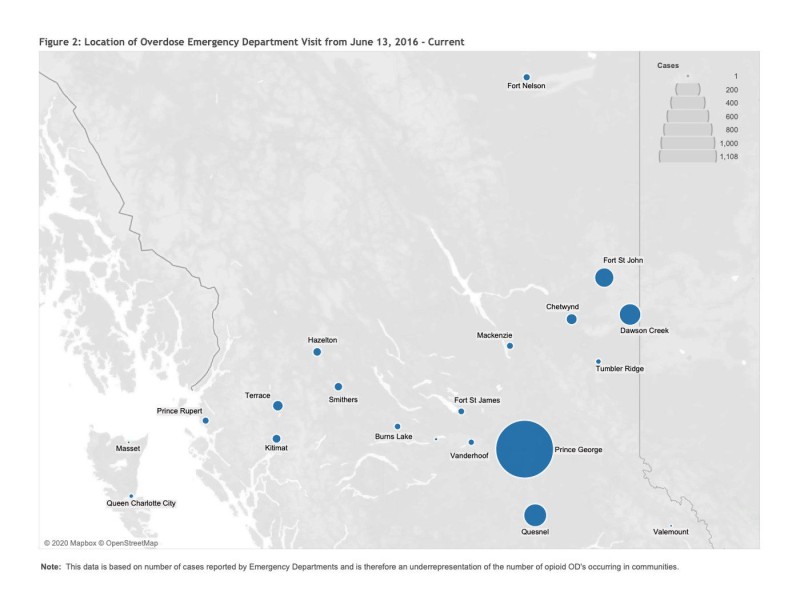
Northern Health has the highest rate of illicit drug overdose deaths in the province, with the Northeast, North Interior, and Prince George particularly hard hit, according to public health officials.
“At a time where some other health authorities might be seeing slight improvement, just slightly, with some decreases in their overdose deaths, we’re actually seeing an increase,” said Northern Health Medical Health Officer Dr. Rakel Kling just prior to the release of the August opioid data. “Which is very troubling.”
August saw the first substantial decline of deaths for toxic drug overdoses – 147 people died – since COVID-19 public health measures were implemented in March. While many areas of the province experienced a decline, overdoses continued to rise in the North, according to the B.C. Coroners Service.
Prior to the pandemic, the number of people dying of overdoses had been reducing from peak levels in 2017 and 2018. Then COVID-19 hit. Isolation drove more people to use alone, and the street drug supply became more toxic. Overdose deaths in B.C. escalated from 73 people in February to around 180 people in each of May, June and July.
In Canada, between January 2016 and March 2020, 16,364 people died of apparent opioid-related deaths. About 90 per cent of people who have died are aged 19 to 59 and around 80 per cent were men.
In B.C., 60 per cent of the 8,091 people who have died since 2010 resided in the Lower Mainland, yet the highest rate of people dying from illicit drug overdoses occurred in the North where a total of 476 people have died (40 people per 100,000 population) as of August 2020. The province as a whole lost 31 people per 100,000 over that span.
Illicit drugs are defined by the B.C. Coroners Service as heroin, cocaine, MDMA, methamphetamine, illicit fentanyl, along with medications not prescribed to the person who overdosed, and combinations of street drugs and prescribed medication.
Fentanyl or its analogues have been detected in about 80 per cent of all illicit drug overdose deaths. Fentanyl is 50 to 100 times more powerful than heroin. Legal fentanyl is a common anesthetic used to relieve pain. Illegal fentanyl is often mixed with other substances, usually without the substance user’s awareness or consent. More than 90 per cent of all overdose deaths have been deemed accidental.
There are a range of reasons why someone might develop a substance use disorder, said Nick Rempel, Northern Health strategic lead for mental health and substance use.
“We know that lived experience or living experience with trauma is a major contributor to substance use and to addiction,” Rempel said. “As well as a myriad of socio-economic factors that play a role, and some genetic components as well.”
The isolation of a rural or remote lifestyle is another risk factor of Northern living, said Rempel.
Throughout the North, few communities have been immune.
From June 2016 through Aug. 20, 2020, Northern Health reported 1,803 overdoses (fatal and non-fatal) in emergency rooms and health clinics across 22 Northern communities, with 984 occurring in Prince George alone. More than 118 overdoses were reported in Dawson Creek, at least 131 in Quesnel, and 77 or more in Fort St. John.
Many communities were listed as having ‘less than five’ overdoses to protect people’s privacy in small rural communities.
As drug overdose deaths increased dramatically during the pandemic, the provincial health officer expanded the range of health professionals who can prescribe opioid replacement treatment to include registered nurses, pharmacists and nurse practitioners, along with, physicians. Treatment can also be accessed by contacting a primary care health professional or calling 811.
Standard practice in Northern Health when interacting with people who may benefit from help with substance use, is to engage them in an alternative opioid treatment and provide take-home Naloxone kits, Rempel said.
Naloxone is an easily injected medication that can reverse an opioid overdose. Almost 800,000 Naloxone kits have been distributed in B.C., with more than 66,000 kits used to reverse an overdose, according to BCCDC.
One modelling study published by BCCDC estimated alternative opioid treatment, supervised injection sites and take-home Naloxone kits prevented more than 3,000 overdose deaths in B.C. between April 2016 and December 2017, with 93 overdose deaths averted in the North.
Naloxone kits can be picked up throughout the province for free from many pharmacies, hospitals, health clinics and agencies.
To find the nearest location, visit www.towardtheheart.com/site-finder
By: Fran Yanor, Local Journalism Initiative Reporter
Source: The Rocky Mountain Goat
Stay connected with local news
Make us your
home page