Fort St. John Hospital operating at over 120 per cent capacity, new data reveals
The Fort St. John Hospital is among seven B.C. hospitals to have operated at over 120 per cent capacity in the 2024-25 fiscal year.

FORT ST. JOHN, B.C. — The Fort St. John Hospital is among seven B.C. hospitals to have operated at over 120 per cent capacity last year.
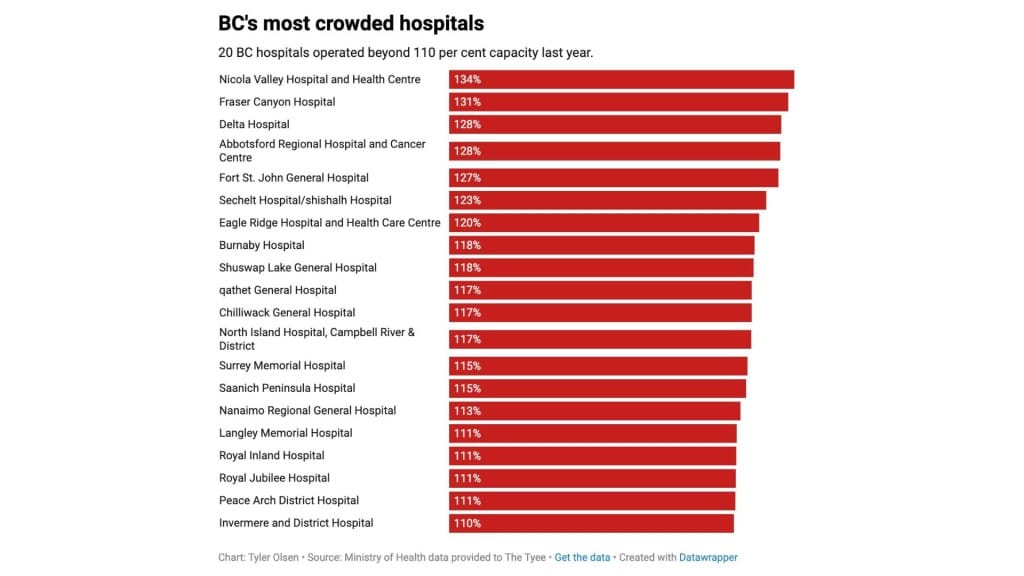
Ministry of Health data provided to The Tyee has revealed Fort St. John Hospital operated at 127 per cent in the 2024-25 fiscal year.
Other facilities joining Fort St. John to operate above 120 per cent capacity included Nicola Valley Hospital and Health Centre, Fraser Canyon Hospital, Delta Hospital, Abbotsford Regional Hospital and Cancer Centre, Sechelt/shíshálh Hospital and Eagle Ridge Hospital.
All seven have operated over capacity each of the last three years.
B.C.’s most crowded hospital in both the 2022-23 and 2024-25 fiscal years was Nicola Valley Hospital and Health Centre in Merritt. Last year, the hospital operated at 133.5 per cent.
When hospitals are overcrowded, patients are placed in so-called ‘surge beds,’ which can be located in hallways, storage areas or other places not designated for full-time, ongoing care.
Latest Stories
The term ‘surge beds’ has only recently become widely used to describe such spaces. Previously, Fraser Health — the province’s largest health authority — called such spaces “inappropriate locations” in internal memos.
In those memos, officials were told care in such locations “is not ideal from a patient or staff perspective” and that “maintaining high hospital occupancy (e.g., over 95 per cent) is associated with longer lengths of stay and higher risk for error and adverse events.”
Many of the province’s biggest facilities operated between 10 and 20 per cent above capacity. Those include Burnaby Hospital, Surrey Memorial Hospital, Langley Memorial Hospital, Chilliwack General Hospital, Nanaimo Regional General Hospital, Royal Jubilee Hospital in Victoria and Royal Inland Hospital in Kamloops. Every day, a combined average of 329 patients in those seven facilities are cared for in makeshift spaces.
B.C.’s health organizations and their leaders have spoken about their work to reduce hospital congestion for more than a decade, for example when Northern Health executive Lisa Zetes-Zanatta addressed over 800 hours of hospital closures across northeast B.C. to Energeticcity.ca.
However, the figures reveal they have been unable to do so.
The challenges are myriad, according to health experts and the province’s own minister of health.
For a decade, officials have spoken about the need to care for more patients out of hospital. That focus often involves the development of home health programs that deliver care to seniors where they live. The goal is to allow people to remain in their homes as long as possible before needing to move to an assisted or long-term care facility.
In an interview with The Tyee, health minister Josie Osborne spoke about the ongoing quest for broader community wellness.
“It’s about modernizing infrastructure and making sure that we’re doing everything possible to reduce those preventable or avoidable hospital visits, to speed up the diagnostics and treatment that people receive, to strengthen care in community so that people stay healthier, they stay independent and they stay at home,” Osborne said.
Additional data provided by the Ministry of Health points to one reason why progress remains elusive.
Since 2018-19, the number of inpatient cases in B.C. hospitals has increased by only four per cent — far slower than the province’s general population and its population of seniors.
But the patients who do arrive are lingering in hospital for much longer. The number of inpatient days has increased by 16 per cent since 2018-19, according to the data provided to The Tyee.
A major part of the challenge lies in the number of patients in hospital who don’t actually need hospital care, but are awaiting other means of care.
Such “alternate level of care” patients account for between 10 per cent and 15 per cent of all acute care users in B.C. Most often, such patients are seniors waiting for space in an assisted or long-term care home. Others may be waiting for care to be organized in their own home or in a rehabilitation facility.
Osborne said the province has made some strides towards addressing the issue, pointing to newly opened long-term care homes, and improved primary care options facilitated by new urgent care centres and pharmacists with the ability to provide expanded care.
In June, the Ministry of Infrastructure announced a new long-term care home had been approved for Fort St. John.
Unfortunately, these efforts have not yet moved the needle.
Stay connected with local news
Make us your
home page






