Code Grey: Systemic Failure in Northern Health

In what some believe to be the aftermath of a global pandemic, there is a significant focus on B.C.’s over-burdened health care system, gaps in which disproportionately affect rural and remote regions, such as the Peace region.
The ICU in Fort St. John has been closed since June 2020, and Chetwynd General Hospital has been forced to close or divert its emergency room over 50 times in the past two years, according to data compiled from Northern Health.
The staffing shortage puts undue pressure on patients and those working in the health care field, culminating in a toxic environment for hospital staff.
While urban areas are just beginning to see the cracks in the system, those in northern and rural communities are quite familiar with the inequities and gaps in care – and have been trying to raise their concerns for years.
Looking for something to do?
Check out our new Events Calendar!
The Peace region is no stranger to shortages of health care workers. In Fort St. John alone, there have been long-term doctor shortages dating back to 1974.
Today, residents in the North Peace region continue to struggle to access essential medical care, while health care workers contend with burnout, mental health struggles, and critically low staffing numbers.
This is part one of Energeticcity’s series Code Grey, where we look to decipher the current state of the health care system in Northeast B.C. by speaking with health officials, local leaders, health care staff advocacy groups and patients. Part two of our series will look at the history of health care in the north.
“We need to acknowledge that our health care system was pretty much in shambles before COVID hit. We need to be brave and ask the questions.”
Fort St. John mayor, Lori Ackerman.
Latest Stories
Mayor of Northeast B.C.’s largest community wants change
Energeticcity is the voice of the Peace. Support our investigative reporting and be the reason we can cover the next story. Give $10 a month today!
Fort St. John mayor Lori Ackerman says she believes the health system in the north really needs attention.
The Fort St. John ICU has been closed since 2020. The hospital reportedly has ICU beds for patients set up in the ER. Ackerman questions if that is the right environment for those patients to be in and if there is enough staff to provide one-on-one care those patients require.

She says that Fort St. John, one of the largest cities north of Kamloops, should not be struggling to keep necessary services accessible to residents.
“To have a hospital that is ten years old now that is struggling to keep essential services open tells you that we’re doing something wrong,” Ackerman said.
“It just makes my head spin and pop. We have a significant population. We’ve got 22,000 people within the city boundaries. That does not include the people that come here for services, which every so often are more because of diversions in other communities.”
“Doing an audit on Northern Health would be specific to the north. But this issue is right across the province and across Canada. If you’re brave and courageous enough to ask uncomfortable questions, people will tell you what the issues are.”
She adds that the pandemic is not what is primarily behind Northern Health’s current crisis.
“We need to acknowledge that our health care system was pretty much in shambles before COVID hit. We need to be brave and ask the questions.”
Local leaders seeking answers
In February 2022, Ackerman, along with other members of the Resource Municipalities Coalition (RMC), took a step towards finding answers to those questions by sending a request for a comprehensive third-party operational audit of the Northern Health Authority to Health Minister Adrian Dix.

The Resource Municipalities Coalition is a group that looks to provide a high quality of life to citizens of resource communities through the “provision of services that ensure safety, education, health, economic vitality and a healthy natural environment.”
Members of the coalition include the City of Fort St. John, the District of Taylor, and the District of Tumbler Ridge.
In the request, the coalition recognized that many requests had been put forth but said it believed an audit was necessary to identify the activities and processes of Northern Health and where there may be gaps in delivering “an effective health care system.”
Coalition members who signed off on the RMC request include Ackerman, Taylor mayor Rob Fraser, Tumbler Ridge mayor Keith Bertrand, mayor of Mackenzie Joan Atkinson, and Fort Nelson mayor Gary Foster.
Ackerman says the minister has yet to respond to the coalition’s audit request.
The RMC’s request for an audit came after a previous audit, requested on November 26th, 2021, by the Peace River Regional District, was denied by the ministry in a letter on February 1st, 2022, despite minister Dix saying he’d be open to an audit just months before.
“Health Authority operations, including at NHA, have been significantly impacted by COVID-19 for the past two years and are currently facing unprecedented challenges caused by the Omicron variant, which is affecting staff and patients. The Ministry of Health does not feel an audit of NHA’s operations is warranted at this time,” the ministry’s letter reads.
Despite the response the PRRD received, the RMC put forth their request, which goes on to detail a proposed fivefold framework for the audit.
First, identify the current level of core services provided by each location and region, and assess and determine gaps that exist within the location and region compared to B.C.’s minimum core service levels for health care.
Second, RMC suggests the auditor should review administration services that each health service delivery area provides by using a mapping structure to determine overlaps, duplications, staffing levels, the effectiveness of organizational structure, and accountability in the context of delivering a “strong, effective, accessible, and sustainable health care system.”
“Perhaps an audit will show some of the gaps in our system. What we seem to be seeing here are these deficiencies in the health care system, and I think the important thing here is to have a look at the health care system throughout Northeast B.C. or all of the Northern health area to see where we can spend dollars more effectively, what are the issues, and how do we cover the gaps?” Fort Nelson mayor Gary Foster said.

Taylor mayor Fraser says he believes one of the issues facing Northern Health is that the authority’s jurisdiction is too large.
“Northern Health has a vast geographic area that they have to cover. The organization is so big that there’s got to be gaps there. We want to understand the service levels across the entire region to see whether or not there are gaps and inequities, where we’re doing things really well, and see if there’s an opportunity to learn from that.”
Northern Health’s jurisdiction and challenges
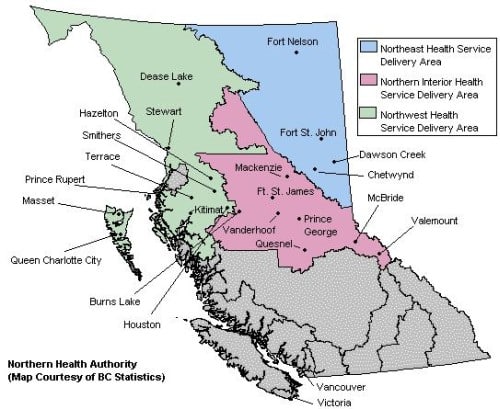
The Northern Health Authority covers over 605,000 square kilometres (over two-thirds of B.C.), making it the largest geographic health region in the province.
NHA’s jurisdiction is comprised mostly of rural and remote communities. In fact, according to data from the RMC, within the NH region, there is only 6.7 per cent of B.C.’s population covering approximately 70 per cent of the land area.
The health authority is split into three health service delivery areas — the Northeast, Northern Interior, and the Northwest. Each of these health service areas has its own administration.
In its 2021-23 service plan, Northern Health laid out the challenges the health authority faces in health care delivery.
The first challenge, according to the health authority, is geography. In Northern B.C, there are many small communities scattered across the large landmass that is the NH jurisdiction.
“The vast geography makes accessing services difficult and complicates the referrals and relationships that exist between practitioners,” the plan reads.
It also notes that many northern communities exist in areas on the other side of the “digital divide” and lack other supporting infrastructure such as affordable public transit, referencing the recent loss of the Greyhound bus system.
Fraser says from his perspective, there has been a deterioration of health care services in the north since the province centralized health care in 2001.
“That’s sort of the crux of the problem is we don’t fully understand [NH] processes. Once we have this audit done, then we would know what we’re dealing with. Right now, we’re making stabs in the dark.”
Mackenzie mayor Joan Atkinson.
RMC’s other recommendations
The coalition’s third recommendation is an assessment of support networks available to health care professionals and support services, which it says can be accomplished by reviewing the accessibility to career and educational development, recognition of diversity based on location, family support, mental health support, and positive work cultures.
Bertrand says from his perspective, a deficiency in Northern Health is their ability to recruit but mainly retain staff as well as allow staff to maintain a work-life balance.
“We’re seeing a lot of agency nurses filling the gaps in a lot of our communities. I’m not sure what it would take for Northern Health to be able to attract and retain them to work for the health authority or not. But it seems like, in my opinion, the agency route seems to be much more flexible and a little bit more able to provide a work-life balance for these nurses.”
Next, the RMC proposes a review of Northern Health policies and processes regarding the recruitment of health care professionals and support staff.
Mackenzie mayor Joan Atkinson says that until municipalities are privy to this information, they’re unsure how to best support recruitment and retention efforts.

“That’s sort of the crux of the problem is we don’t fully understand [NH] processes. Once we have this audit done, then we would know what we’re dealing with. Right now, we’re making stabs in the dark,” Atkinson said.
“We have some very credible information from the people who are working in the trenches, the clinicians, nurses and staff. But as far as Northern Health policies and processes, we don’t know, and that’s why we want that audit.”
Finally, the coalition urges the auditor to review and identify current and emerging trends that challenge the delivery of a solid and effective health care system in the Northern Health Authority’s jurisdiction.
Chief operating officer for Northern Health’s northeast division, Angela De Smit, says the health authority undergoes regular external audits through Accreditation Canada.
“These are individuals, health individuals that come from all across Canada that come to us and look at what we’re doing and provide us with recommendations for opportunities for improvement and [tell us] what we’re doing well.”
De Smit adds that if a facility can’t be accredited, it can’t be funded by the province.
“We are turning almost vulnerable people into vulnerable people. If I had to wait to go down for this test, the reason I’m having this test might be worse by the time I get it done.”
Fort St. John mayor Lori Ackerman
Audit framework based on feedback from community members
Recommendations within the RMC audit request are based on a January 2022 Health Care Advocacy report completed by the coalition, which, through discussions with member councils in the development of its 2021-2023 strategic plan and discussions with local health care staff, found seven key gaps and anomalies.
The RMC found that the level of service that residents in rural and remote communities are not the same provided to residents of larger urban centres.
In fact, the RMC states that the level of service provided by Northern Health differs “significantly” in each community.
The coalition says the administrative structure of service delivery is different in each community within the health authority.
It says access to increased levels of service — such as referrals for testing, diagnostics, or specialists — varies throughout the health authority, but overall is considered to take too long or be insufficient.
When Ackerman had a referral for a diagnostic procedure, and a technician went on sick leave, she says she had to get another referral just to get the test she needed.

“They said to me, you have to go back to your doctor to get a referral. I asked doesn’t my cancellation here just kind of trigger something, and then my doctor can refer me [elsewhere?] They said no, I have to go back to my doctor and get another requisition,” Ackerman recalled.
She says she was headed to Vancouver for work and asked for the referral to be sent to a facility there but was then informed that she’d only be able to be tested within the Northern Health jurisdiction.
“We don’t have an efficient, direct flight to Prince George. If I needed to go there in an efficient way, I’d have to drive. That’s four and a half to five hours down, and the same thing on the way back, or I’m staying overnight. When I’m going down to Vancouver for business, I can slip into one of the hospitals down there, get it done, and I’m finished.”
Ackerman says that while she has the luxury of having a functional vehicle and the confidence to drive wherever, not everyone needing to access medical services has that ability.
“We are turning almost vulnerable people into vulnerable people. If I had to wait to go down for this test, the reason I’m having this test might be worse by the time I get it done,” Ackerman pointed out.
RMC discussions also identified that the recruitment of medical professionals is inconsistent regionally and “results in unreliable distribution of general practitioners, nurses and other professionals across the region.”
“Health care is a high priority for the Northern Rockies because it affects all our citizens. One of the biggest challenges with health care is the number of people in the health care industry. We’re short of nurses, doctors, lab techs, and not just in the Northern Rockies or in British Columbia, but in fact, all across Canada,” Foster said.
He adds that this is a huge problem in smaller communities such as Fort Nelson because a staff shortage has a more profound impact.
“So, for instance, we lost both our lab techs in the Northern Rockies. Without lab techs, we couldn’t do blood work, this represents a huge problem in a small community because that essentially means you can’t do a quick blood test.”
Foster’s comments were echoed in Northern Health’s 2021-2023 strategic plan
Due to the health authority serving primarily smaller, spread-out rural communities, small facilities and services are common in the health authority’s service offerings. However, these facilities and services can be difficult to sustain.
“The departure of a single practitioner, for instance, can have a significant impact on many northern communities,” NH’s plan states.
Other challenges the health authority stated include human resources, transient resource-sector populations, poorer health statuses among residents, and a rising “burden” of chronic diseases
According to the RMC, recruitment practices also include requests for financial support by local governments without transparency when it comes to what those processes are, how the money is used and the return on investment.
The coalition also notes that the compensation model for doctors is inconsistent, makes recruitment more difficult, and creates a culture of “desirable and undesirable” community postings.
After several months of consultations and reviewing “various reports, studies, and documents on health care developed by provincial and federal governments as well as physicians,” the coalition identified three areas of concern: accessibility to effective health care, recruitment and retention, and mental health and addictions.
There is significant overlap between these concerns, which the RMC says further complicates the determination of effective solutions.
“Not having enough RNs and NPs means patient needs may go unmet, and [patients] may have to wait longer for care. Working long hours to cover vacant shifts increases the risk of medical error and can lead to burnout, illness and injury, and backfilling shifts at overtime rates or with agency nurses is more expensive.”
Carol Bellringer, 2018 auditor general
Staffing challenges in the North
It is no secret that the Northern Health authority — and other health authorities across the province — have been struggling with the recruitment and retention of health care staff.
A 2018 audit by the Auditor General of BC found that Northern Health was not doing enough to recruit and retain nurses effectively.
“As of April 1, 2017, Northern Health was short 121 full-time-equivalent registered nurses, approximately 15 per cent of its rural and remote RN workforce and at least 5.9 full-time-equivalent nurse practitioners. It was able to fill approximately half of its vacant shifts with nurses who work on a casual basis and existing nursing staff, sometimes at an overtime rate. The remaining shifts went unfilled or were covered by agency (contracted) nurses at a higher hourly wage,” wrote Carol Bellringer, auditor general at the time.
Bellringer added that the shortage of nurses has disastrous effects on patients and health care staff.
“Not having enough RNs and NPs means patient needs may go unmet, and [patients] may have to wait longer for care. Working long hours to cover vacant shifts increases the risk of medical error and can lead to burnout, illness and injury, and backfilling shifts at overtime rates or with agency nurses is more expensive.”
Chief operating officer for Northern Health’s northeast division, Angela De Smit, says that the health authority has a “robust workforce sustainability strategy.”

“We’ve contacted over 144 internationally educated health care professionals that live here in the Northeast. Lots come here because they have taken or are enrolled in the Northern Lights College Health Services Management Administration program,” De Smit said.
She adds that the health authority hires about a hundred new graduates each year.
“Some of the successes are that we’ve built back and will have almost filled all of our emergency room department positions [in Fort St. John] by the end of October. I believe there’s a part-time position that will remain unfilled. We’re now 50 per cent filled back up with our ICU,” De Smit said.
While Northern Health has made further efforts to recruit more nurses in recent years, the Peace region continues to face a severe staffing shortage. There are factors that are out of the hands of the health authority, such as weather conditions and geography; however, others remain well within its control.
During a recent visit to the Energetic City, vice president of the BC Nurses Union, Adriane Gear, says members in Fort St. John are reporting increased negative patient outcomes because there aren’t enough nurses to provide care to those in the community.

“In the emergency room, for example, their baseline ratios are two nurses to 16 patients or one to eight. In any other part of the province, you’re going to see a ratio of one to three or one to four,” Gear explained.
De Smit says that in the Northeast, the health authority doesn’t measure in ratios.
“What we look at is our statistics in terms of what is the acuity of patients that are coming into the facility and what is the reasonable amount [of staff] because there’s always peaks and valleys,” she explained.
“That’s why at times, we do pull staff because, for the last three days, we were fine. We had staffing that was appropriate to care for the number of patients in there. And then maternity might drop down to two mums and babes, and the emergency department spikes. So we say, okay, how do we support the emergency department? Because right now, they have an increase of patients.”
In September of 2022, the BCNU held a town hall meeting with nurses in Fort St. John who highlighted issues they face in their workplace, such as severe staffing challenges and a lack of respect from the health authority.
“We have two types of people in the health care system who live in our communities — the people who use the system and the people who work the system. The people who work the system are telling us something completely different with respect to what it’s like to work in Northern Health than what the administrators of Northern Health are telling us.“
Rob Fraser, Taylor mayor
North Peace nurses feel disrespected, unsupported
Gear says that local nurses don’t feel listened to or supported by Northern Health.
“They certainly acknowledge that some of their immediate managers are good people trying the best that they can do. But, generally speaking, they do not feel supported or listened to by the health authority,” Gear said.
She adds that because nurses are not covered by whistleblower protection, they are unable to speak out publicly due to the threat of losing their jobs.
Gear says many nurses feel they are unable to bring up genuine health and safety concerns and practice standard issues because of a fear of retaliation.
“If someone brings a patient safety concern forward, they’re considered to be stirring the pot or a troublemaker. So what’s happened is that nurses who historically have brought forward patient care issues are now saying, why would I bother? Nothing happens.”
She says this leads to more nurses considering vacating their positions because they don’t feel confident in the level of care they’re providing.
“They don’t feel good about what they’re doing as a nurse. They cannot provide the care that patients deserve or require.”
Rob Fraser, the mayor of Taylor, says that during consultations with health care workers for the RMC Health Care Advocacy report, he saw a disconnect emerge.

“We have two types of people in the health care system who live in our communities — the people who use the system and the people who work the system. The people who work the system are telling us something completely different with respect to what it’s like to work in Northern Health than what the administrators of Northern Health are telling us.”
Atkinson, the mayor of Mackenzie, also noted a disconnect after speaking to health care workers in her community, who she says aren’t feeling supported.
“They’re not having good conversations with administration. I don’t know if they don’t fully recognize the crisis that the clinicians feel that they’re in, but there have to be some more open conversations so that we can get to the root of what’s working and what isn’t working and why we’re having such a hard time retaining staff, especially nurses, in our community,” Atkinson said
Fraser says there appears to be a cultural gap within the health authority, with some employees mentioning a toxic work environment.
“The nurses can tell you about the toxic environment, the general administrative workers cleaning staff, the workers in the food department, they’re the ones that you know can really identify the specific causes of the toxic environment,” Fraser said.
He says that nurses also spoke of concerns surrounding basic training, staffing levels, and cross-department training.
“[Nurses mentioned] being able to train between departments. So making sure that if nurses ever have to go work in emergency that they’re trained in the emergency department because you can imagine a nurse going to the emergency department. If she’s not trained, she’s going there because they don’t have enough people. If there are not enough people there, she’s gotta try to make decisions on her own without being adequately trained. You can see how that must put enormous stress on people,” Fraser said.
According to the BCNU, Northern Health has also allegedly changed the model of care, requiring all primary care nurses to be generalists, meaning they must learn and be competent in all complexities of the different areas of nursing.
“The primary care has changed here. So where they would have a specialty in seniors care, diabetes care, mental health, or pediatrics, now they’re being asked to be a generalist in everything,” BCNU president Aman Grewal explained.

Grewal says this is can be a massive strain on nurses’ mental health and also takes them away from the work they’re passionate about.
“You don’t become an ICU nurse because somebody told you that’s what you have to do, you do it because you have that in you and that adrenaline. There’s that draw to certain things,” Grewal began.
“I was drawn to pediatrics, and I was drawn then to pediatric emergency, so those were my specialties. Then it evolved, and it was diabetes care as well. Nurses have passions for certain things, and now they’ve had that taken away.”
Gear says the change has led nurses to feel disrespected by Northern Health.
“Nurses need to be respected and acknowledged for the unique skill set they bring, for the specialized training and experience they acquire. There should not be this position of a nurse is a nurse is a nurse,” Gear said.
Chief operating officer for the northeast division of Northern Health, Angela De Smit, denies that this is a new change, stating that because the north is comprised primarily of rural and remote communities, most don’t have enough staff to always practice in specialty areas.
“Nurses come out as generalists. They have med-surg training, maternity training, pediatric training, and that’s what the north really likes is the fact that they are generalists and they’re well rounded,” De Smit said.
“This is always the case where staff float back and forth to different units depending on their comfort level and what our needs are to minimize service disruptions.”
Grewal says if steps aren’t taken by the health authority to address these issues, the nursing shortage will continue to escalate, causing the health care system to “crumble.”
“What [Northern Health] needs to do is talk to the members. Talk to me and talk to my team. We’ve got labour relations officers, servicing, all sorts of different people that they could be talking to. We need to come to the table and see how we can figure out how to solve this for our members.”
“But, the most important thing is to listen to the members and see what it is that they want because they are your workforce.”
“My question back to them is how are we not reaching you? We’re doing it electronically, on paper, in meetings, in Zoom. I do walkabouts in the facility. It’s two ways in terms of them reaching out to help us understand how we’re not communicating with them.”
Angela de Smit, Chief operating officer, Northern Health Northeast Division
Communication break-down
Nurses aren’t alone in feeling ignored by Northern Health. According to a 2021 engagement survey by Doctors of BC — which saw 20 doctors who work at the Fort St. John Hospital respond — 35 per cent of those doctors said they feel like the health authority doesn’t value their contributions, while another 45 per cent indicated that they felt neutral.
When it comes to the Fort St. John Hospital, 50 per cent of survey respondents say they feel as though the facility values their contributions, while 30 per cent say they don’t feel that way. 20 per cent answered neutrally.
In the same survey, 65 per cent of the FSJ hospital doctors said senior leaders don’t seek physician input when setting health authority goals and 60 per cent say that leader decision-making is not transparent to physicians. Another 30 per cent felt neutral.
60 per cent indicated that senior leaders don’t communicate the health authority’s plans to physicians in a clear and timely way. An additional 15 percent said they felt neutral.
De Smit says she’s surprised at these statistics, stating that physicians have numerous opportunities to communicate with Northern Health.
“I regularly had twice weekly meetings that were Zoom calls that all physicians could attend to keep them informed, ask them questions about how to best deliver services. We had them for each community,” De Smit said
She says there are also regular local medical advisory committee meetings, a weekly medical digest detailing information relevant to physicians, as well as regular presentations De Smit facilitates to present new information and allow doctors to ask questions.
“My question back to them is how are we not reaching you? We’re doing it electronically, on paper, in meetings, in Zoom. I do walkabouts in the facility. It’s two ways in terms of them reaching out to help us understand how we’re not communicating with them.”
“In the context of health care, we would often rely on expected standards that are put in place by the ministry of health, expected standards that may have been through policy, standards of care, it can even just be best practice if it relates to depending on the subject matter.”
BC Auditor General’s office
What an audit may look like
An audit of Northern Health — or any health authority — would likely vary depending on who performs the audit and what subject matter is involved.
According to the BC Auditor General’s office, an independent office of the legislature, a broad, comprehensive audit of a large organization wouldn’t necessarily be how they would address an issue. Instead, the office would examine particular aspects of the organization.
A representative for the BCAG says during a performance audit, the office usually looks at what is known as the three E’s of operations — effectiveness, efficiency, and economics.
“The economic piece is more about how the organization is procuring materials, effectiveness is usually ‘did they achieve what they were expecting to achieve,’ and efficiency is ‘did they achieve it without significant duplication or waste,’” the representative explained.
When auditing an organization such as a health authority, the office says it follows the Canadian standard on audit engagements.
“It’s a CPA standard. It requires us to really establish what we term is kind of a framework of measurement, and that would include our audit objectives. So that’s the overall statement that we would be concluding against. It has to be something that we can say that it is, or it isn’t, or it is with some exceptions.”
The office says that to draw a conclusion, it must set up audit criteria that would establish benchmarks of what the office would expect the organization being audited to have in place.
“In the context of health care, we would often rely on expected standards that are put in place by the ministry of health, expected standards that may have been through policy, standards of care, it can even just be best practice if it relates to depending on the subject matter.”
The BCAG says extensive research goes into establishing criteria which are then peer-reviewed.
During an audit, the office communicates with the organization in a “no-surprises” approach, even communicating findings so deficiencies can be addressed through the audit process.
Once the audit is finished, the office then develops recommendations for improvement and releases a public report, which is then tabled with a select standing committee.
The committee would then call witnesses from the government side, discuss findings and request an action plan.
“We need to have our emergency rooms opened 24/7. We live in a community that’s supported by the resource industry. People are out driving logging trucks, harvesting trees, and carrying out mining activities. So, pretty high-risk jobs that could result in needing medical attention if something went wrong and if the hospital is on diversion because we don’t have enough staff to keep that hospital open, then that is a major concern.”
joan atkinson, mayor of mackenzie
Health care accessibility is top of mind for local leaders
While each mayor detailed concerns specific to their community, they were all in the same vein — a lack of access to essential care services.
“We’re starting to hear of health care issues across the breadth of the province, but for us, it started in the Northeast. The availability of health care services in all of our municipalities, we felt, was starting to wane,” Taylor mayor Fraser stated.
“We felt it wasn’t fair just to complain, so we contacted some nurses and doctors and put together a community report amongst all our communities in our councils to see what our concerns were,” Fraser said, referring to RMC’s Heath Care Advocacy report.
Mayor of Tumbler Ridge, Keith Bertrand, says if the request for an audit goes through, he hopes it will uncover some information to improve services being offered in rural and remote communities like his.

“When it comes right down to it, Tumbler Ridge is basically a transport center. We’re looking at other options through transport. It’s very appreciated that BC ambulance put a helicopter in service through Prince George. It’s been used a few times over the last couple of years, so it’s definitely appreciated.”
Atkinson says staffing challenges in her community of Mackenzie have had a significant impact on keeping the hospital open. She says that from August 17th to 24th, 2022, the Mackenzie ER was on diversion for three of those nights from 11 p.m. to 7 a.m., with the closest hospital located in Prince George — almost 2 hours away.
“We need to have our emergency rooms opened 24/7. We live in a community that’s supported by the resource industry. People are out driving logging trucks, harvesting trees, and carrying out mining activities. So, pretty high-risk jobs that could result in needing medical attention if something went wrong and if the hospital is on diversion because we don’t have enough staff to keep that hospital open, then that is a major concern.”
“People are losing their lives in this province because of staffing shortages and inefficiencies. Everyone’s working as hard as they can with what they have, but we think that this audit would better give a better understanding of what’s broken and what we can fix, working collaboratively with both the clinicians and administration,” she said.
In our series Code Grey, we look to decipher the current state of the health care system in Northeast B.C. by speaking with health officials, local leaders, health care staff advocacy groups and patients. Part two of our series will look at the history of health care in the north.
Energeticcity reached out to the Ministry of Health on numerous occasions but was unable to obtain a statement by the time of publication.
Those who wish to share their stories about being a patient in Northeast B.C. can do so by emailing Spencer Hall at spencer@energeticcity.ca.
Stay connected with local news
Make us your
home page







