Evan Saugstad: My prostate, my journey – making a decision (part 2 of 8)
Evan Saugstad’s series discussing his journey with prostate cancer continues.
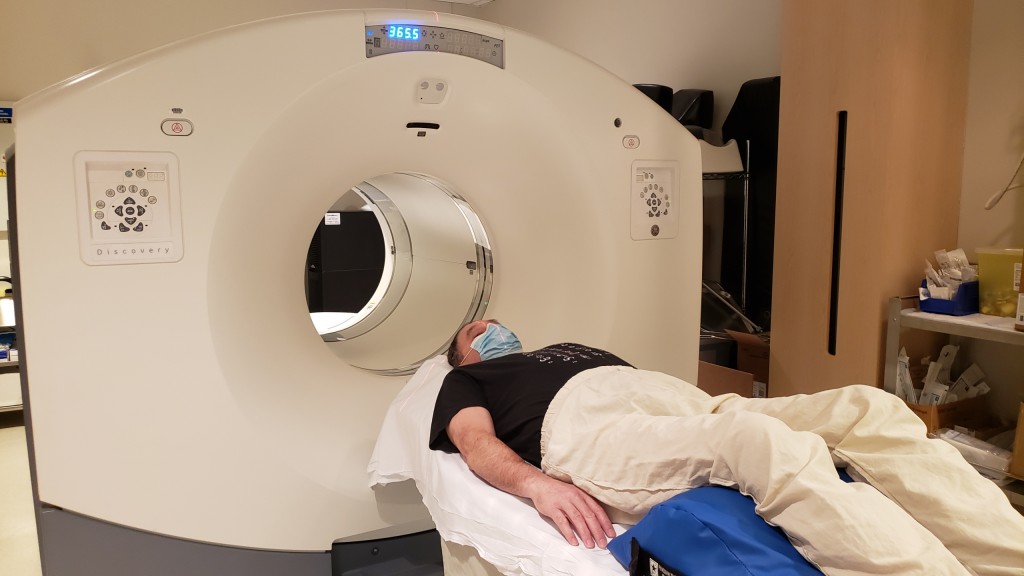
FORT ST. JOHN, B.C. — Although September is known as Prostate Cancer Awareness Month, I have chosen to tell my prostate journey for Movember, Men’s Health Month. I have also chosen to discuss subjects that are not normally found in our local newspaper; one’s personal health, one’s sexual health and one’s cancer.
Movember is the month where the largest percentage of donations are made in support of curing men’s cancers and improving our health. Please support Movember.
If the discussion of a man’s body parts, or medical procedures or men’s sexual health offends you, then skip the rest of this. Just be assured I am still alive, still kicking and still adjusting to life with cancer and cancer treatment.
Local News Straight
to Your Phone
Download our app today!
Available on Android and iOS devices
With my PSA (prostate-specific antigen) at 18.32 in March 2019, and my Drs. suggesting no more watchful waiting, off I go to find out more about my cancer.
Back to Vancouver General Hospital (VGH) in April for a full body bone scan. Good news, no cancer detected in any of my bone mass.
Over to the BC Cancer Agency to discuss treatment options. Dr. suggests two.
Surgical removal (radical prostatectomy) which takes 3 – 4 hours of surgery, or a combination of hormone (androgen deprivation) treatment for six months, followed by 5 to 6 weeks of external beam radiation therapy (EBRT), which is akin to having multiple x-rays, followed by the insertion of radioactive beads around my prostate.
Latest Stories
Dr. carefully explains the pros and cons, the possibility and likelihood of side effects and longer-term implications.
Hormone therapy reduces the size of the prostate and lowers one’s androgen levels. A smaller prostate is easier to treat with radiation beams and lower androgen levels slows the growth of cancerous cells. Of note, androgens are manufactured in the testicles and control the development of male physical traits, such as a deep voice, and facial hair.
EBRT is the process where radiation is beamed into the body targeting the prostate, once per day for up to six weeks. This virtually “cooks” the prostate, rendering it non-functional. Once completed, radioactive beads are inserted, surrounding the prostate and remain in place as the body dissolves them.
Both processes could be completed in either Vancouver area hospitals or in Prince George.
Armed with a whole bunch of literature and online references to read, I head back to my urologist for a more fulsome discussion about surgery.
He and his team still use the “old fashioned” approach, a retropubic prostatectomy. They would try to employ “nerve sparing” surgery, which entails leaving one or both sets of nerve bundles in place. These nerves are immediately adjacent to the prostate and control erectile functions.
Surgery would entail making a 3-inch vertical incision above the pubic bone, detachment of the bladder to allow access to the prostate, removal of the prostate and associated lymph nodes in the immediate vicinity, reattachment of the bladder, insertion of a catheter through the penis and then all stitched up. 3 to 4 hours in the operating room under a general anesthetic. 1 to 2 days in the hospital, then 2 weeks with a catheter and 6 weeks of no strenuous exercise or lifting and I should be good to go.
Time has come to face reality, make a decision and move on, as doing nothing has been ruled out.
Lots of thoughts. What are the risks? What does one wish to live with? What will I be satisfied with? What are the side effects? Allot to think about and discuss with Karen.
Now, must try to digest all this information and the statistics. Both radiation and surgery options have risks, and no Dr. can say for certain just how close to normal your body will be after removing or obliterating your prostate.
Incontinence issues (leaky valves) is a bit greater with surgery as compared to radiation. It could take up to a year for these valves to either regain their composure, or for one to understand just what the full extent of the impairment is. Normal bladder control usually returns within a few weeks, but in some cases, it doesn’t. One can speed up the process by immediately beginning Kegel exercises to strengthen one’s urinary valves.
Erectile dysfunction severity (what was hard, will now be softer) can be about the same for both. Surgery results in immediate impairment, while radiation may take a few years. Post operation, there will be changes and there will be effects that can range from never achieving another erection to partial erections that can still allow for intercourse. As with the incontinence issues, it can take up to a year for nerves to recover or repair themselves and find out just what the level of impairment. With practice, and concentration, one can still achieve an orgasm after either method, but both will result in no ejaculations (dry) and both will result in complete infertility.
Surgery has greater risks for infections and anesthetic complications. Radiation has greater risks for rectum irritations and bowl infections.
Doctors can’t say for sure just how we will be affected after the operation. In general, the older one is, the more likely it is to have incontinence and erectile dysfunction issues. And as always, the more experienced the surgeon, the less likelihood there will be complications.
Making a long story a bit shorter, I chose to stick with my urologist and a retropubic prostatectomy, as that is how they operate. I could have found another urologist elsewhere and had a laparoscopic surgery (multiple small incisions using a small remote camera to guide the surgeon) or gone to a VGH surgeon and had robotic-assisted laparoscopic surgery (a surgeon guides a robot) but chose not to. All three of these methods have similar success, complications and side effect ratios and all depend upon the skill and expertise of the surgeon and their team.
Please support Movember as Men’s Health Month, give generously, and help fund cancer research. If you are over 40 and have not had a PSA test, ask your doctor to prescribe one. If you wish to skip that part, book your own appointment, pay $35, and get your own. It could save your life.
Evan, and always willing to talk about my journey and answer any questions you may have.
Stay connected with local news
Make us your
home page
Letters to the Editor
Letters to the Editor should be exclusive to Energeticcity.ca. Include your name, address and daytime phone number. Keep letters to 500 words or fewer. Letters may be edited for length and clarity. To submit a letter by e-mail to contact@energeticcity.ca.






